ADDONS / GENERAL NEUROLOGY
Raeder paratrigeminal syndrome
Updated on 14/10/2024, published on 03/03/2024
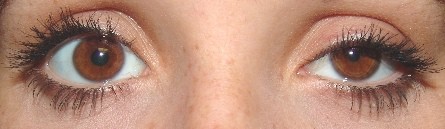
- Raeder paratrigeminal syndrome (RPS) is a rare neurologic disorder characterized by unilateral oculosympathetic paralysis (postganglionic Horner syndrome) + ipsilateral sensory and/or motor abnormalities in the distribution of the trigeminal nerve (usually the first branch)
- also known as Raeder syndrome or paratrigeminal neuralgia
- can be confused with Horner’s syndrome; however, in Raeder syndrome, trigeminal nerve irritation and preserved facial sweating help to establish the correct diagnosis
- it is most commonly caused by lesions in the middle cranial fossa
Anatomic notes
- the dilator pupillae muscle is innervated by the sympathetic nervous system and causes mydriasis
- the efferent part of the reflex arc contains three neurons: central, preganglionic, and postganglionic
- central sympathetic neurons are located in the hypothalamus
- they terminate on preganglionic neurons in the intermediolateral nucleus in the spinal segments C8-Th2
- axons from preganglionic sympathetic nuclei enter the sympathetic trunk via white ramus communicans and ascend upward to the superior cervical ganglion
- oculomotor fibers have their center at the T1 level, and sudomotor fibers at the T2-3 level
- axons from preganglionic sympathetic nuclei enter the sympathetic trunk via white ramus communicans and ascend upward to the superior cervical ganglion
- postganglionic nerve fibers (third-order sympathetic neurons) arising from the superior cervical ganglion are part of the periarterial carotid plexus
- sudomotor fibers for the maxillary and mandibular regions run along the ECA
- oculomotor and sudomotor fibers for the medial forehead run along the ICA through the carotid canal
- sudomotor fibers turn laterally after exiting the carotid canal and are therefore not affected together with the oculomotor fibers in Raeder syndrome
- oculomotor fibers accompany the ophthalmic branch of the CN V to enter the orbit through the superior orbital fissure
- preganglionic lesions cause anhidrosis on the entire ipsilateral side of the face; the manifestation of postganglionic lesions depends on whether the plexus around the ICA or ECA is involved

Etiology
- ICA abnormalities (e.g., aneurysm, dissection, inflammation, congenital abnormalities, fibromuscular dysplasia, trauma)
- middle cranial fossa and cavernous sinus tumors
- inflammation (e.g., chronic sinusitis, Tolosa-Hunt, etc.)
- trauma (e.g., basilar skull fracture, Gasserian ganglion injury, gunshot wound)
- iatrogenic
- idiopathic
- Raeder syndrome has also been associated with cluster headaches, SUNCT syndrome, ophthalmic herpes zoster, migraine headaches, and Lyme disease
Clinical Presentation
- unilateral headache with or without facial pain or sensory deficit + postganglionic Horner syndrome (without impaired forehead and face sudomotor activity)
- pain (often severe and lancinating) is located in the distribution of the trigeminal nerve, which is often periocular or retroorbital; pain may also involve the maxillary division
- trigeminal nerve involvement may also include other sensory abnormalities, including decreased facial sensation and corneal reflex
- Müller muscle of the superior eyelid, the inferior sympathetic lid retractor, and the dilator pupillae muscles are affected ⇒ ipsilateral ptosis and miosis
- less common symptoms
- additional cranial nerve involvement
- conjunctival hyperemia (chemosis)
- trigeminal motor abnormities
Diagnostic evaluation
- physical examination
- anisocoria more pronounced in the dark (with dilation lag) + semiptosis due to impairment of the oculosympathetic pathway
- ipsilateral sensory deficit in the head and face
- careful neurological examination, including extraocular movements, corneal reflex, and facial sensation, should detect other cranial nerve involvement
- brain CT/MRI + vascular imaging (CTA/MRA)
- angiography should exclude ICA aneurysm
- digital subtractive angiography may be added to characterize the potential aneurysm
- angiography should exclude ICA aneurysm
- pharmacologic testing may help confirm the postganglionic lesion
- however, many authors have recommended omitting pharmacologic testing and proceeding with neuroimaging of the entire oculosympathetic axis in patients with clinically diagnosed Horner syndrome due to the variable sensitivity and specificity of the pharmacologic testing
- 1% or 0.5% apraclonidine (an alpha-1 and alpha-2 adrenergic receptor agonist)
- under normal circumstances, the alpha-2 agonist effect predominates in the presynaptic membrane
- in the presence of oculosympathetic denervation, supersensitivity allows the postsynaptic alpha-1 agonist effect to predominate, leading to pupil dilation of the affected eye with mild constriction of the normal pupil; test confirms Horner syndrome
- under normal circumstances, the alpha-2 agonist effect predominates in the presynaptic membrane
- cocaine inhibits the reuptake of norepinephrine, perpetuating a sympathetic adrenergic response
- 10% topical cocaine will cause dilation in the normal eye but will not cause the same degree of dilation in the affected eye
- one drop of topical cocaine should be placed in each eye and checked after 15 minutes; repeat twice if the first test is negative
- failure to dilate the abnormal pupil suggests oculosympathetic denervation but does not further localize the lesion
- hydroxyamphetamine
- topical 1% hydroxyamphetamine can distinguish between pre- and postganglionic lesions in the oculosympathetic pathway
- hydroxyamphetamine leads to the release of norepinephrine from the third-order neuron junction; in the case of paratrigeminal neuralgia, the pupil of the affected eye would fail to dilate
- equal dilation of the pupils after hydroxyamphetamine testing (in cocaine or apraclonidine confirmed Horner syndrome) would be suggestive of a first or second-order neuron disorder
The International Headache Society criteria for the diagnosis of Raeder Syndrome include
- constant, unilateral headache
- imaging evidence of underlying disease of either the middle cranial fossa or of the ipsilateral carotid artery
- evidence of causation demonstrated by both of the following:
- headache has developed in temporal relation to the onset of the underlying disorder
- headache has either or both of the following features:
- localized to the distribution of the ophthalmic division of the trigeminal nerve, with or without spread to the maxillary division
- aggravated by eye movements
Differential diagnosis
- ICA aneurysm (compressive syndrome)
- carotid artery dissection
- parasellar and skull base tumors
- parasellar tumors
- propagation of nasopharyngeal tumors
- skull base tumors propagating through the carotid canal [Uzuner, 2017]
- middle fossa meningioma
- inflammatory disorders (such as Tolosa-Hunt syndrome)
Therapy
- the treatment depends on the underlying etiology
- antithrombotics (most commonly antiplatelet therapy) or CAS for dissection
- embolization of the aneurysm
- resection of the tumor
- if no intracranial etiology is found, treatment is aimed at symptomatic relief
- analgesics, steroids, intensive vitamin B therapy
- patients should avoid triggers (e.g., vasodilators, particularly alcohol) during the active phase of the disease