NEUROIMAGING / NEUROSONOLOGY
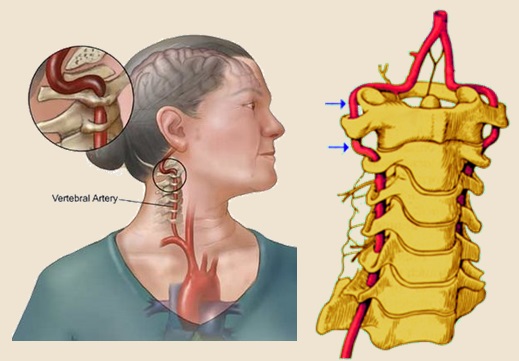
Bow Hunter’s syndrome
Updated on 14/06/2024, published on 09/12/2021
Definition
- Bow Hunter’s syndrome (also known as Rotational vertebral artery occlusion syndrome) is a symptomatic vertebrobasilar insufficiency caused by mechanical compression of the vertebral artery (VA) at the level of the atlanto-axial joint during head rotation within the normal physiologic range
Etiopathogenesis
- rotation and head tilt lead to vertebral artery compression, disrupting flow in the posterior circulation
- location of compression:
- at the level C1/2 (atlantoaxial type) – during contralateral head rotation [Sorensen, 1978]
- at the level C2-6 (subaxial type) – associated with ipsilateral head rotation [Miele, 2008]
- combined disability
- etiology
- congenital skeletal abnormalities
- atlantoaxial hypermobility
- bone abnormalities, including large osteophytes
- vascular malformation
- vertebral instability
- fibrous streaks (often observed during surgery)
- aberrant course of the vertebral artery
- compression by the thyroid cartilage
Clinical presentation
- clinical symptoms are provoked by unilateral head rotation (combined with retroflexion) and disappear when the head is returned to the neutral position
- transient vertigo
- visual disturbances
- drop attack or syncope
- TIA / vertebrobasilar stroke
- symptoms usually occur with concomitant contralateral vertebral artery pathology (hypoplasia, stenosis/occlusion), indicating that the dominant vertebral artery is compressed
Diagnostic evaluation
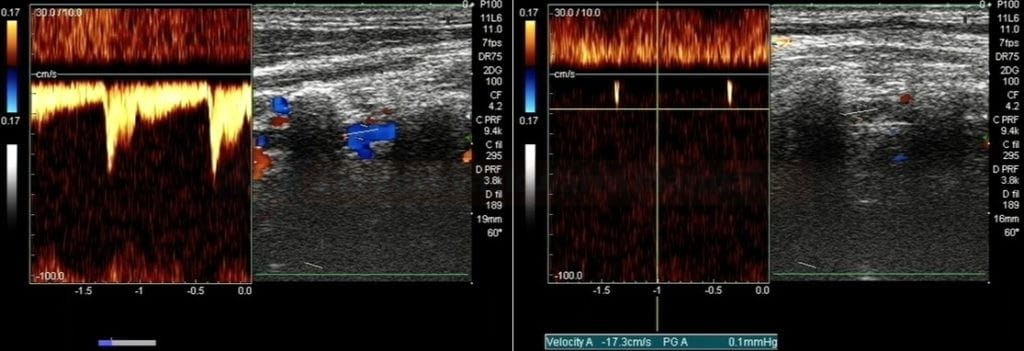
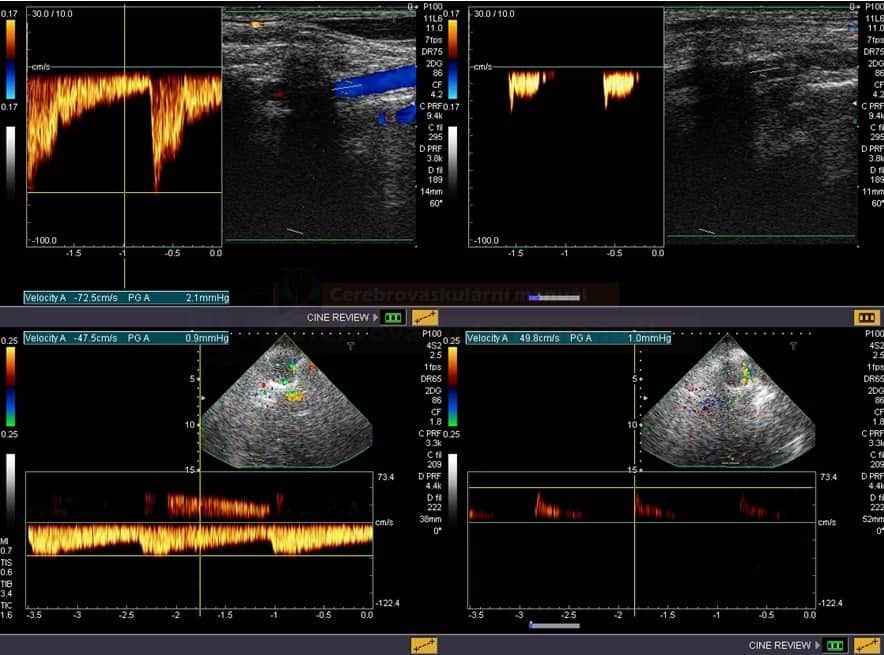
Dynamic Doppler ultrasonography
- ultrasound may detect flow in the vertebral artery during head rotation combined with tilt (according to the patient’s reported provocation position)
- reliable, easy to perform method that can be used for both screening and follow-up
- it is useful to add TCCD examination, especially for type 2 (subaxial) diagnosis, where head rotation to the examined side makes extracranial examination difficult
- evaluation of the V4 segment helps to determine the hemodynamic significance of dynamic compression
Standard and dynamic cervical spine X-ray
- detects morphologic abnormalities in the spine
- dynamic images assess spinal instability
- functional views should not be performed on trauma patients without strict instructions from a clinician
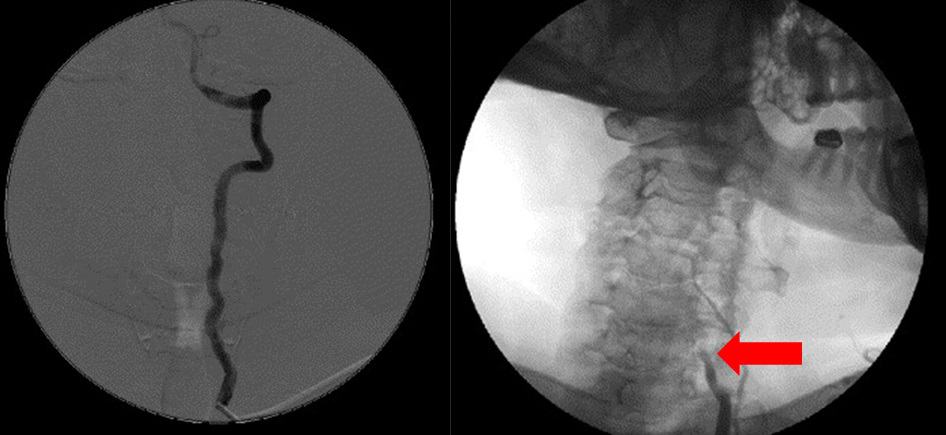
Dynamic DSA
- DSA is performed at rest and then during the movement, provoking typical symptoms
- it identifies the side and level of the compression (which can range from the C6 entrance to the C1/2 level)
- DSA, however, cannot determine the exact cause of the compression
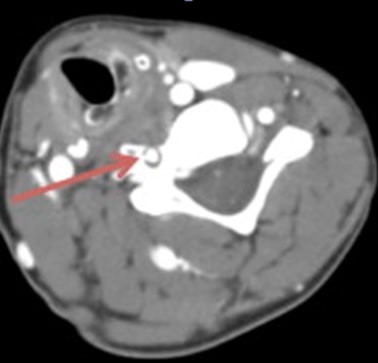
Dynamic CTA
- able to identify both the exact location and cause of the compression
- involves higher radiation exposure compared to other methods
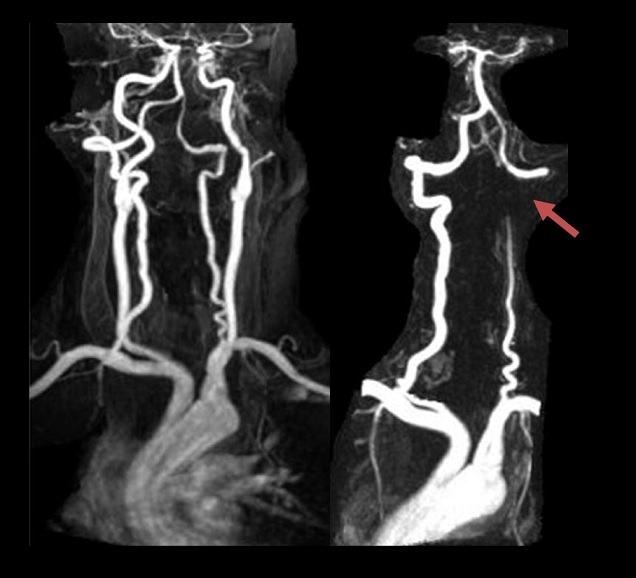
Dynamic MRA
- MR angiography can serve as a reliable and less invasive diagnostic tool, potentially replacing DSA
- it is suitable for confirming adequate postoperative decompression and monitoring recurrence (Anaizi, 2013)
Management
Treating this condition requires careful consideration, as the long-term prognosis of untreated forms remains unknown
- the conservative approach is recommended in most cases
- for severe posterior fossa symptoms, surgical solutions are available
- vertebral body fusion (for atlanto-axial instability)
- deliberation of the vertebral artery course (anterior/posterior vertebral artery decompression)
- if the flow in the contralateral AV is restricted, e.g., by severe proximal stenosis, then primary stenting of this stenosis should be considered