ISCHEMIC STROKE / ETIOPATOGENESIS / INFECTIOUS VASCULOPATHIES
Neuroborreliosis and stroke
Updated on 10/03/2024, published on 22/02/2024
Introduction
- Lyme disease (borreliosis) is the most common anthropozoonosis; the typical vector of borrelia is the tick Ixodes ricinus
- ticks, larvae, and nymphs are found in forested areas, parks, and suburban gardens from March to mid-November
- Lyme disease is transmitted through tick bites, usually within 24 hours of attachment
- Borrelia burgdorferi (BB), Borrelia garini (BG), and Borrelia afzelii (BA) belong to the order Spirochetales
- Borrelia burgdorferi sensu lato (BG and BA) predominate in Europe, Borrelia burgdorferi sensu stricto in the USA
- Borrelia burgdorferi sensu lato (BG and BA) predominate in Europe, Borrelia burgdorferi sensu stricto in the USA
- involvement of the nervous system is reported to occur in 10-15% of patients with Lyme disease (Halperin, 2015)
- stroke due to CNS vasculitis is a rare complication of the disease, single case reports or small series have been published (Garkowski, 2017)
- borreliosis-associated vasculitis should be excluded in all patients with vasculitic pattern on imaging and multiple ischemic lesions, especially in those living in endemic areas
- remove attached ticks as quickly as possible, preferably with tweezers
- do not remove the tick with unprotected fingers; rubber gloves are preferable
- do not apply pressure to the tick; remove it with a rocking motion from side to side and a gentle pull
- a circular motion is inappropriate, as is the use of oils or greasy creams
- on the other hand, it is advisable to rub the wound with antiseptic
- after removing the tick, treat the area with an antiseptic again

Pathogenesis
Tissue damage occurs in borreliosis due to:
Direct effect of Borrelia
- direct cytotoxic effects are seen in erythema chronicum migrans (ECM) and other skin conditions, synovitis, arthritis, myocarditis, and endocarditis.
Autoimmune process
- especially important in neuroborreliosis
- mediated by the autoimmune action of T lymphocytes against neurons and glial cells
- cross-reactivity of anti-Borrelia antibodies with myelin sheaths and neuroglia is also significant
Vasculitis
- commonly affects spinal roots, peripheral nerves, and muscles
- vasculitis affecting cerebral arteries is rare, but possible
Neuroborreliosis and stroke
- if parenchymal and vascular imaging suggest vasculitis, borreliosis should be excluded among other causes, especially in patients exposed to ticks or who live in areas with high prevalence of tick-borne diseases [Garkowski, 2017]
- vasculitis is presumed to be caused by the inflammatory response to the spirochetal infection
- symptoms of stroke in neuroborreliosis are similar to those of stroke from other causes
- risk factors include:
- delayed diagnosis and treatment of Lyme disease
- severe systemic inflammation
- involvement of large blood vessels by vasculitis
- the presence of traditional cardiovascular risk factors
- without proven vasculitis, the causal relationship between stroke and neuroborreliosis is unclear and other significant stroke etiologies must be excluded
| clinical and radiological signs of stroke + vasculitic pattern of vascular imaging |
| + |
| confirmation of neuroborreliosis (according to EFNS guidelines) |
| + |
| exclusion of other etiologies (including other vasculitides!!) |
Clinical presentation
Early localized stage
- occurs days to weeks after a tick bite when borrelia multiply in the skin
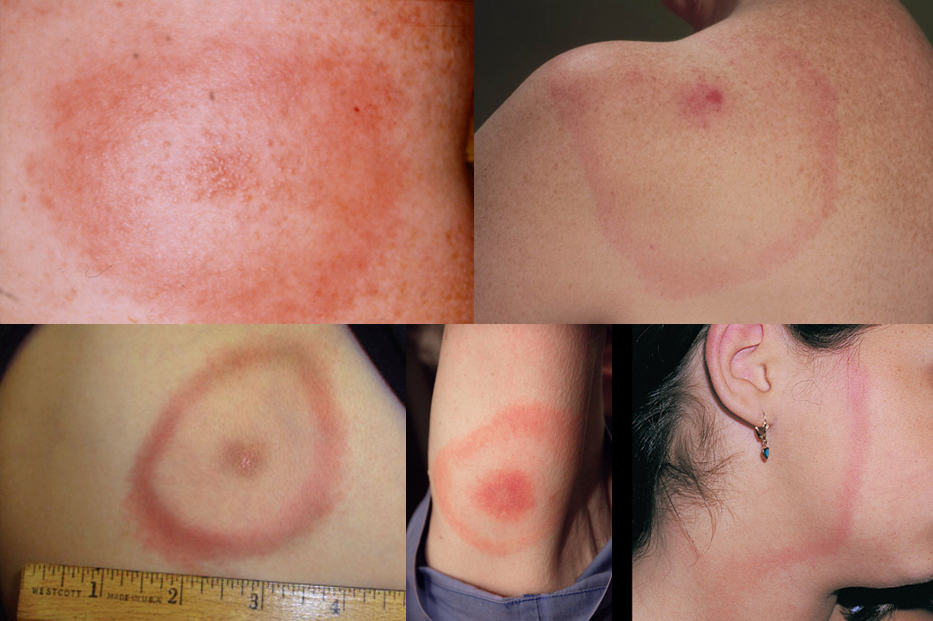
- the most typical manifestation is erythema (chronicum) migrans (EM or ECM)
- appears within 4-5 weeks after a person has been bitten by an infected tick
- a characteristic red expanding bull’s-eye rash, with a central clearing surrounded by a red outer ring
- it often gradually enlarges and may reach sizes of up to several inches in diameter
- a hallmark sign of Lyme disease, although not all individuals with Lyme disease develop this rash
- general flu-like symptoms (subfebrile, fatigue, malaise, muscle, and joint pain, possibly regional lymphadenopathy) may occur
- neurological involvement at this stage is less common but can include mild meningitis or cranial nerve palsies
- early recognition and treatment of EM are crucial for preventing progression to later stages of Lyme disease
Disseminated stage
|
Early disseminated stage (2-12 weeks)
|
Neurological Symptoms
|
|
Cardiac symptoms
|
|
Skin Symptoms
|
|
ENT Symptoms
|
|
Late disseminated stage (> 6 months)
|
|
Neurological symptoms
|
|
Other symptoms
|
Diagnostic evaluation of borreliosis
Specific antibodies
- specific antibodies (ELISA + Western blot confirmation) in serum and CSF
- low sensitivity during the first weeks of infection
- a positive result does not necessarily indicate the presence of bacteria in the organism – it may only indicate contact of the patient with the antigen of the infectious agent that led to the subsequent antibody response
PCR
- false-positive and false-negative results in serum and especially in CSF, are common
- PCR can be used in the early stages when there is no antibody response and in immunosuppressed individuals
- testing is not recommended in the late stages
CSF analysis
- cytology
- lymphocytic pleocytosis, typically around 10-1000 / mm3 of elements
- normal findings are rare in neuroborreliosis
- elevated protein levels (reflecting disruption of the blood-brain barrier and inflammation in the central nervous system)
- detection of specific antibodies (ELISA or Western blot) + assessment of intrathecal synthesis
- the problem is a low sensitivity in the early stage and, conversely, their persistence after treatment
- oligoclonal bands
- indicate intrathecal antibody production
- not specific for neuroborreliosis, can be found in other inflammatory diseases
- electron microscopy (ELM) – low sensitivity/specificity
- CSF analysis may be repeated during treatment to monitor response to therapy and guide further management decisions
Imaging methods
- MRI
- often non-specific findings
- multifocal T2 periventricular/subcortical hyperintensities in the white matter (mostly in frontoparietal regions, sometimes in basal ganglia, thalamus, and brainstem)
- lesions may be present in the corpus callosum (differential diagnosis of MS)
- cranial nerve enhancement
 [Hildernbrand, 2009]
[Hildernbrand, 2009] - leptomeningeal enhancement
- CNS vasculitis is manifested by an ischemic lesion on DWI + vasculitic pattern on MRA/CTA (irregularities of the vessel lumen with occlusion or segmental narrowing or dilatation)
- CT – usually a normal finding in neuroborreliosis, ischemic lesions can occur in CNS vasculitis
Other tests
- EMG, evoked potentials, EEG
- Holter ECG, echocardiography
- skin biopsy, etc.
Management
- neuroborreliosis is typically treated with antibiotics
- the choice of antibiotic and duration of treatment depend on factors such as the severity of the symptoms, the stage of the infection, and the patient’s medical history
- commonly used antibiotics include doxycycline, ceftriaxone, and penicillin
- intravenous administration of antibiotics may be necessary for more severe cases or if the infection involves the central nervous system
- if stroke due to CNS vasculitis is suspected, corticosteroids and antiplatelet therapy should be added
- use treatment regimens from evidence-based guidelines established by medical societies specializing in infectious diseases or neurology
Post-Lyme disease syndrome (PLDS)
- difficulties (fatigue, joint and muscle pain, cognitive impairment, paresthesia) persisting for > 6 months after standard treatment of neuroborreliosis
- recurrent or persistent infection must be excluded
- prolonged antibiotic therapy has no effect in PLDS